For years, patients and many doctors assumed that a colonoscopy was a colonoscopy. Patients who had one seldom questioned how well it was done. The expectation was that the doctor conducting the exam would find and cut out any polyps, which are the source of most colon cancer.
But a new study, published today in The New England Journal of Medicine, provides a graphic illustration of how wrong that assumption can be, gastroenterologists say. The study, of 12 highly experienced board-certified gastroenterologists in private practice, found some were 10 times better than others at finding adenomas, the polyps that can turn into cancer.
One factor distinguishing the physicians who found many adenomas from those who found few was the amount of time spent examining the colon, according to the study, in which the gastroenterologists kept track of the time for each exam and how many polyps they found.
They discovered that those who slowed down and took their time found more polyps.
. . .
The Rockford study was preceded by other signs that colonoscopies are by no means foolproof. But as problems have been pointed out, they have all too often been met with disbelief among doctors, Dr. Rex said.
The first indication that colonoscopies were not as effective as widely believed came with two studies, one in 1991 and a larger one, in 1997, in which patients had two colonoscopies on the same day. Those studies showed that doctors were missing 15 to 27 percent of adenomas, including 6 percent of large adenomas.
Then, in the last few years, two studies of so-called virtual colonoscopies, which use a CT scan to view the colon, found that the rate of overlooked adenomas in traditional colonoscopies was even higher. Patients in those studies had traditional and virtual colonoscopy on the same day. Traditional colonoscopies missed 12 to 17 percent of the large adenomas detected in the virtual colonoscopies. But many doctors dismissed those findings, saying — if they believed them at all — that they applied to other doctors, not to themselves, Dr. Rex said.
Dr. Schoen, for one, said he was a believer. The conclusions of the adenoma detection studies were reinforced, he said, by studies finding that colonoscopies missed not just polyps but actual cancers.
That finding emerged from studies testing ideas about how to prevent polyps, like taking beta carotene or calcium pills or sticking to a low fat, high-fiber diet.
The patients in all the studies had at least one adenoma detected on colonoscopy but did not have cancer. They developed cancer in the next few years, however, at the same rate as would be expected in the general population without screening.
. . .
The study by the group in Rockford suggests a way to improve colonoscopy: by slowing down. “If you rush things, you miss things,” Dr. Schoen said.
That happens in part because reimbursement rates for colonoscopies have fallen in recent years, and some doctors are doing the exams faster than ever, Dr. Schoen and others say.
“I have heard of people who do it in 30 seconds,” Dr. Schoen said. “Whoosh, and it’s out.”
 CEO of drug company Eli Lilly. Source of image: online version of WSJ artcle cited below.
CEO of drug company Eli Lilly. Source of image: online version of WSJ artcle cited below.

 Source of book image:
Source of book image:  Source of book image:
Source of book image:  Source of image: online version of WSJ article cited below.
Source of image: online version of WSJ article cited below. 
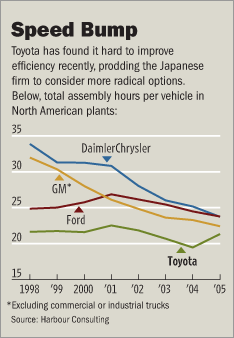 Source of graph: online version of WSJ article cited below.
Source of graph: online version of WSJ article cited below. Source of book image:
Source of book image: 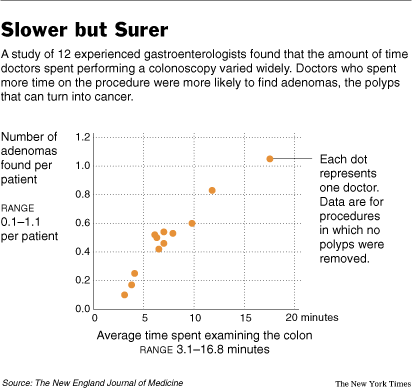 Source of graph: online version of the NYT article cited below.
Source of graph: online version of the NYT article cited below.